Families of cancer patients raise infection concerns with first minister
 BBC
BBCCharly Bisset is still alive thanks to a stem cell transplant performed by doctors at Glasgow's Queen Elizabeth University (QEUH) hospital, which helped her beat leukaemia.
But six years on, the 14-year-old says she doesn't trust the hospital.
Charly still has questions about life-threatening infections she contracted during her treatment there, and the serious health issues she'll have to cope with for the rest of her life.
Charly's dad Mark says the public inquiry investigating problems at the hospital is not going to give patients and families the answers they are looking for.
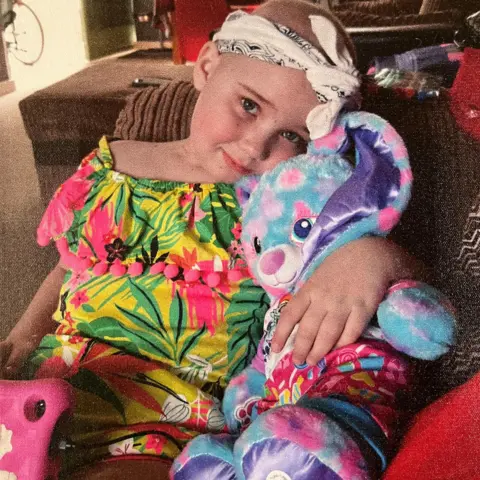 Mark Bissett
Mark BissettThe £840m QEUH campus, which opened in 2015, has been at the centre of a long-running controversy over claims that bacterial and fungal infections were linked to the hospital environment, particularly the water and ventilation systems.
Families of cancer patients who contracted infections while undergoing treatment at QEUH met first minister John Swinney on Thursday.
Swinney has said he will "urgently" look at calls to investigate the long-term impacts of medications given to patients because of water and ventilation problems at the hospital.

Charly, from Peebles, was diagnosed with acute lymphoblastic leukaemia in 2019, three weeks before her seventh birthday.
After the cancer failed to respond to initial treatment in Edinburgh, she was transferred to the QEUH in Glasgow.
She was admitted to the adult hospital because the child cancer wards were closed after a series of infections there.
Charly remembers being put in strict isolation ahead of total body irradiation – radiotherapy throughout her whole body - to suppress her immune system before a bone marrow transplant from a donor.
"I would wake up, take my meds, take my blood, hook me up to IVs, drips, you name it," she says.
"I was hooked up to everything. You just think, yep, this is normal."
The public inquiry has heard evidence that children including Charly were given precautionary antibiotics because of concerns that the hospital's water and ventilation systems posed an elevated risk of infection to those with low immunity.
"I remember I was on a lot of meds," says Charly.
"It was about 50 meds in the morning and it was so hard to keep them down because you were so sick you just couldn't keep them all down at once.
"You weren't allowed to drink the water, you had filters on the taps. But you just think that's normal because you don't know."
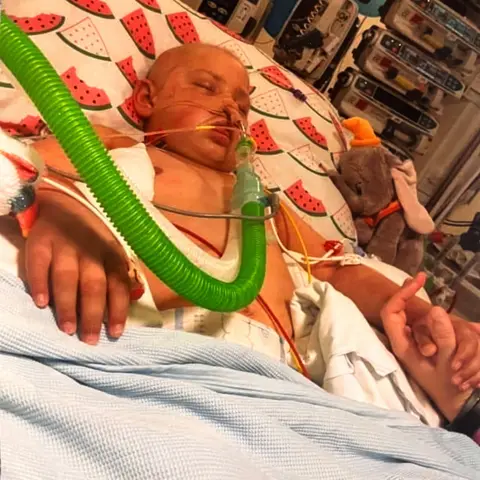 Mark Bissett
Mark BissettCharly's stem cell transplant was successful, but in the days that followed she developed life-threatening sepsis and was admitted to intensive care.
Her dad Mark feared the worst.
"It's a nightmare," he says. "It's a living hell.
"I said the worst ever news is getting told that your kid has cancer but then to be watching their life fading away in front of your eyes is even worse.
"It wasn't just once or twice, it was four times we were sitting there and called the family in to say goodbye."
As well as being treated for a severe viral infection in her bloodstream, Charly was given powerful anti-fungal drugs after tests suggested aspergillosis – a fungal lung infection caused by mould spores in the air.
Mark says that, at the time, this was not explained to them.
"It was always referred to as fungal infections," he says.
"And then when she ended up in intensive care I heard the nurse saying on a handover to the evening shift that Charly has got high levels of aspergillus.
"I just questioned the nurse about, 'she's got what'?"
Mark says he went home and researched aspergillus and how it was contracted.
"After I read what it was, that it come from mould and building work, I'm like, 'well that can't be happening in a hospital'."
Mark believes that spores could have come from the ventilation system in the building.
In Ward 4B, where Charly had been treated, he took photos of the empty isolation room next door, which was sealed off for repairs.
In 2024, the public inquiry heard evidence from microbiologist Dr Christine Peters that aspergillus mould had been found in air sampling in Ward 4B and the children's cancer wards as early as 2015.
 Mark Bissett
Mark BissettAfter seven weeks in intensive care, Charly was discharged to Ward 4B and eventually went home in November 2019. Doctors kept her on the anti-fungal medication until the following March.
Mark is concerned that their prolonged use has had a long-term impact on Charly's health.
"It's not a long-term drug yet Charly was on them for months," Mark says.
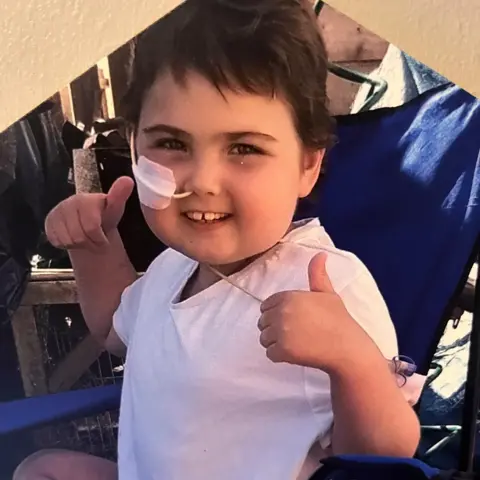 Mark Bissett
Mark BissettCharly, who was seven when she was in hospital, says the impact on her as she gets older has been "really overwhelming".
Although she is now cancer-free, she has been left with adrenal insufficiency, which Mark believes may have been caused by anti-fungal treatment.
This means her body can't produce essential hormones, and it affects her every day.
"If I fall over, if I hit my head, pass out or break a bone, I need this injection within half an hour or my body starts to shut down and it can kill me," she says.
Although Charly was unaware of the problems at the hospital when she was younger, she now dreads going back for check-ups.
"I hate going there because I just don't feel safe," she says.
Mark says that while the public inquiry is tasked with investigating what was wrong with the building's ventilation and water, it won't look at individual cases like Charly's.
He says another investigation should look into the long-term health issues for patients.
Although he believes the hospital is safe for the vast majority, certain patients are still at higher risk there, he says.
"I couldn't be any more grateful for the transplant doctor and intensive care staff that brought her back to life," he says.
"But the people running that hospital are putting lives at risk on a daily basis."
'Challenges' from the hospital building
The first minister said he appreciated the "candour and views" expressed by the families during the meeting.
He said: "I want to recognise the profound, unimaginable pain and loss they have experienced, and I appreciate the inquiry has reopened longstanding and deeply painful wounds.
"I made clear that today is the start of a wider discussion with the government to help families get the answers they need.
"We will continue to do everything in our power to help them get the answers they rightly deserve, and families will have an important part to play in the new Safety and Public Confidence Oversight Group."
A statement from NHS Greater Glasgow and Clyde said it had faced challenges linked to the build quality of the hospital since it opened in 2015, and the board acknowledged the impact this has had on patients.
"Where historical issues have been identified, comprehensive programmes of remediation and assurance have been undertaken. Safety is actively managed everyday and we continue to monitor performance including the use of approved equipment to ensure wards remain safe for our patients," the statement said.
"This includes thorough testing of the water and ventilation to provide additional safety assurance, particularly for our vulnerable patients.
"While we cannot comment on individual patient cases due to confidentiality, consultants are always transparent with families about medication provided.
"As part of the ongoing Scottish Hospitals Inquiry, a number of matters are being investigated, and we are fully committed to supporting the inquiry in its considerations of the planning, design, construction, commissioning and maintenance of the QEUH/RHC."
NHSGGC said it remained focussed on "providing safe, high quality care for all patients" and the statement called on anyone with concerns to come forward.
