Universal flu vaccine: How scientists are closing in on the virus's 'weak spots'
 Getty Images
Getty ImagesWhile current flu shots need to be updated each season, scientists are finding new ways to make vaccine that could last much longer and cover more strains.
Each year, roughly a billion people around the world catch the flu. You'll know if you've got it – it can knock you out for a week or more with a fever, fatigue, headaches and a cough. It leaves millions of people each year unable to work and sadly claims the lives of between 290,000-650,000 people in a typical year.
It's a miserable disease – and, unfortunately, there's no guarantee that if you catch it one year, you go through the same ordeal the following year. Influenza is a wily virus, constantly shapeshifting to get around humans' immune defences.
"That's why you have to get a flu shot every year," says Nicholas Heaton, a professor at the Duke University School of Medicine in North Carolina, US. Seasonal flu vaccines prevent many deaths and serious illnesses each year, but they are imperfect. Their effectiveness typically tops out around 60% and can dip well below that in years when the vaccine's formula isn't a good match for the virus that is actually spreading among humans.
But what if you didn't have to get a new shot every year? Heaton's lab, and others around the world, are trying to answer that tantalising question. They're developing so-called "universal" flu vaccines, which aim to offer better, broader and more durable protection than current seasonal vaccines. The idea is to "cover more strains or make the shot last longer", Heaton says. "Or, hopefully, both."
There are currently about a dozen such vaccine candidates moving through the clinical trial process and many others still in earlier stages of development, according to an initiative that tracks next-generation influenza vaccine development.
It's a "pretty amazing collection of projects", says Julie Ostrowsky, a research scientist at the University of Minnesota's Center for Infectious Disease Research and Policy, in the US, who works on the tracking project. But it is a complex challenge, she says. "It's not going to happen overnight."
Here's how scientists are taking a stab at the problem.
An ever-changing enemy
The term "the flu" is a bit misleading. Influenza is not a single entity, but many different viruses circulating between people and animals. And these viruses are constantly evolving, allowing them to stay one step ahead of human immune systems. "Flu varies a lot," Ostrowsky says. "It's just a constantly moving target."
 Getty Images
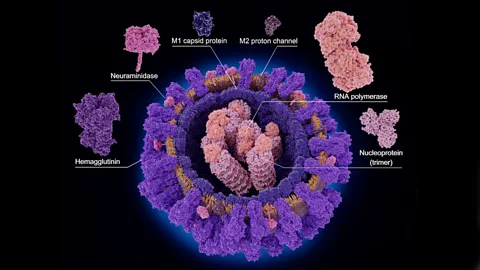
Getty ImagesSome of the shapeshifting components are proteins on the surface of each virus called haemagglutinin and neuraminidase. When you're exposed to influenza, your immune system recognises these proteins and responds in kind, fighting off infection by creating antibodies that bind to them. But the viral proteins are hardly sitting ducks. There are 18 varieties of haemagglutinin and 11 varieties of neuraminidase, which can mix and match to create different flu subtypes, such as H1N1 and H3N2. The viral genes that create these proteins also rack up mutations, resulting in new forms of the virus, splitting into clades and sub-clades.
A mutation here or there may not be enough to outsmart the immune system. But over time, the changes accumulate enough that the body's immune defences are rendered out of date, forcing them to play catch-up. That's why it's so difficult to formulate the flu shot each year. Public health officials and vaccine makers are, in effect, trying to predict the future, making their best guesses about how the virus will change and which specific strains will circulate in the season ahead.
To do so, the World Health Organization (WHO) convenes an international group of experts to pore over reams of data on where influenza is spreading and how it's evolving. Last time they printed all this data, they racked up a 10cm thick stack of double-sided papers, says Wenqing Zhang, from the WHO's department of Epidemic and Pandemic Threats Management.
Each February, the WHO's expert group meets to create recommendations for shots used in the Northern Hemisphere, where flu season typically starts around October. In September, they do the same for the Southern Hemisphere, where flu season typically starts around April.
But a lot can change after these predictions are made. In the 2025-2026 season, for instance, flu outbreaks have been occurring around the world caused by H3N2 subclade K influenza viruses, which weren't even on the WHO's radar in February 2025. "At that time, there was no clade K virus yet," Zhang says, so there wasn't a recommendation to tailor vaccines accordingly.
Despite the surprise, preliminary data out of the UK suggest this year's shots are nonetheless protecting against severe illness and hospitalisation for subclade K, and they seem to work particularly well among children. But the sudden arrival of subclade K shows that influenza can "give us a surprise at a time", often when we don't anticipate it, Zhang says.
To get a leg up on influenza, some scientists are trying to develop shots that train the immune system to recognise and respond to parts of the virus that don't change, rather than those that do.
"There are a few weak spots that the virus has," says Florian Krammer, who is working on universal flu vaccine design at the Icahn School of Medicine at Mount Sinai in New York, US. One is a specific section of the haemagglutinin protein on the influenza virus' surface.
Think of haemagglutinin a bit like an ice cream: a cone base, with a scoop of ice cream on top. The flavour on top can change easily, but the cone is fairly constant. Traditional seasonal vaccines prompt the body to make antibodies that target the ice cream scoop, but Krammer's team is trying to stimulate an immune response against the cone instead.
To do so, they introduce the body to haemagglutinin proteins with familiar cones but unfamiliar flavours of ice cream on top. The immune system, searching for something it knows, zeroes in on the familiar portion – the cone – and directs antibodies toward it. In 2020, Krammer's team published a preliminary study demonstrating that a vaccine candidate based on this technique can generate a broadly effective immune response in people. His team has continued to fine-tune their approach in the years since and plans to move forward with additional human testing this year.
 Getty Images
Getty ImagesHeaton's team is also trying to coax the immune system into responding to parts of the virus that stay the same from strain to strain. They created a vaccine candidate that introduces the body to more than 80,000 variations of haemagglutinin. When confronted with so many different forms of haemagglutinin, the immune system essentially gets overwhelmed. Unable to process all the differences in the changed portions, it instead pays attention to the fixed parts of the protein, Heaton explains.
His team reported promising preliminary data on this approach in a 2024 study, but they are yet to begin human clinical trials.
Researchers at Stanford University unveiled a different approach in February 2026 that they hope will not only help to protect against flu, but also the common cold, coronaviruses such as the one that causes Covid-19 and even particles that cause allergies. Their approach – tested only in mice so far – involves a nasal spray that releases a concoction of molecules designed to mimic the way our immune cells communicate with each other. This awakens white blood cells in the lungs called macrophages, keeping them alert to any infection that might try to enter the respiratory system. The spray's effect lasted for three months and reduced the amount of pathogen intruders by 100-to-1,000-fold, the researchers say. They have, however, still to test the approach in humans.
Other laboratories are working on different types of universal vaccines. Some are trying to get the immune system to pay more attention to neuraminidase, another protein found on the surface of the influenza virus, which does not mutate as quickly as haemagglutinin. Some are trying to stimulate T cells, immune cells with long memories that may be able to recognise and kill infected cells regardless of viral strain. Others are experimenting with new vaccine technologies and formats, such as nasal vaccines meant to stop the virus at the point it actually enters the body.
Getting ahead of surprises
While the methodologies are different, the goal is the same across the board: creating a shot that doesn't depend on the good luck of a good match and instead protects against many different flu strains. Some flu viruses are already circulating in the human population and so are largely responsible for the seasonal spikes in the disease that occur each year. When an entirely new version of the virus appears that is infectious enough, it can lead to a pandemic, as was seen with the H1N1 swine flu pandemic in 2009. More flu viruses still circulate in animals – they are common in birds, but they can infect many different mammals. When these flu viruses pass from animals to humans, they are known as zoonotic. (Read more about how bird flu became an animal pandemic in this article by India Bourke.)
 Getty Images
Getty ImagesA truly universal vaccine would offer "protection against any influenza A or B subtype, any strain, no matter if it's pandemic, zoonotic, or just a seasonal influenza virus," Krammer says. "Universal means everything."
While Krammer believes such a vaccine is scientifically possible, it's a decidedly ambitious target, one that would require lots of time, commitment and funding – resources that are not guaranteed in the current climate of scepticism, he says.
Not all scientists are so bullish about universal vaccines, though. "I hate this term," Heaton admits, in part because he feels it overpromises on what even a greatly improved flu shot could do. A more realistic description, he says, is a broadly protective shot that may not completely block every form of the flu under the Sun, but that nonetheless protects against many more strains than current seasonal shots do.
Can AI fix the flu vaccine?
While they're waiting for the flu holy grail, scientists haven't stopped improving seasonal flu shots. "We're not just relying on this very aspirational, off-in-the-distance model of a universal vaccine," Ostrowsky says. "We've got other things that can productively be done in a shorter-term timeline."
Some steps have already been taken on that front, like approving extra-potent shots with quadruple the haemagglutinin dosage for older adults whose immune systems weaken with age. Other scientists are trying to improve the strain selection process itself.
More like this:
• Are you a flu superspreader?
• The viruses hiding in our DNA
• Should you always treat a fever?
Regina Barzilay, a professor for AI and Health at the Massachusetts Institute of Technology in the US, designed an AI system that combs through vast amounts of influenza data to land on the best possible option for upcoming seasonal jabs – similar to what the WHO's flu vaccine board does yearly, but with enhanced analytical power that could outperform the WHO's recommendations, according to a 2025 paper.
While Barzilay isn't advocating for AI to replace humans, she says public health officials could incorporate such a model along with the data and projection tools they already use.
A true universal flu vaccine – the kind of thing you'd get once and never have to think about again – is a long way off, if it will ever arrive at all. But real progress is possible in the meantime, Heaton says.
"I would not be surprised," he says, "if we have an improved influenza vaccine in the five- to 10-year horizon."
--
If you liked this story, sign up for The Essential List newsletter – a handpicked selection of features, videos and can't-miss news, delivered to your inbox twice a week.
For more science, technology, environment and health stories from the BBC, follow us on Facebook and Instagram.
