Racism and 'poor' staff relationships factors in maternity care failings, report finds
 Getty Images
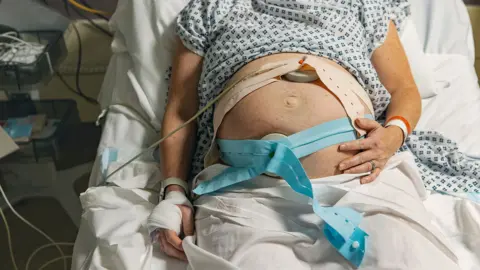
Getty ImagesMaternity services in England are failing "too many" families, with problems "at every stage" of the maternity journey, an interim report has found.
Racism, staffing and accountability issues were among six factors identified by Baroness Amos, who is leading a government-commissioned review.
More than 8,000 people have so far submitted evidence, with Baroness Amos meeting more than 400 families.
Health Secretary Wes Streeting has promised to act on her final recommendations, which are due in April.
 PA
PAIn her interim report, Baroness Amos centred her findings on six key areas. Issues found included:
- Services depleted or stopped because of capacity pressures, with stretched antenatal wards and delivery units resulting in delays to admissions and the use of community midwives in delivery units impacting safety
- "Poor relationships" between team members, including obstetricians and midwives. Racist and bullying behaviour of senior clinicians was not always dealt with by management
- Structural racism and persistent inequalities leading to "notably higher risk of adverse outcomes" for women from black and Asian backgrounds and women from more deprived areas. Discrimination against disabled women, Muslim families, refugee and asylum women and LGBT families was also reported
- A lack of compassion and transparency when baby loss and harm occurs, which can lead to mothers wrongly blaming themselves, compound trauma and impede opportunities to learn from mistakes
- Care being delivered in outdated and dilapidated buildings, in some cases compromising clinical care. Bereavement spaces were insufficient or non-existent in some trusts
- Staff reporting maternity units did not have enough personnel to provide safe care
Baroness Amos said in a statement that it was "clear from the meetings and conversations I have had with hundreds of women, families and staff members across the country, that maternity and neonatal services in England are failing too many women, babies, families and staff".
 Reuters
ReutersFailures within the system have been known about, and reported on, for years. The BBC has spent more than a decade speaking to bereaved and harmed families following poor care at Morecambe Bay, Shrewsbury & Telford, East Kent, Nottingham, Leeds and a number of other NHS Trusts, gathering evidence of failing maternity services.
Orlando Davis died in September 2021, aged 14 days, after staff at Worthing Hospital in Sussex failed to spot his mother had developed hyponatremia, a lower than normal level of sodium in the bloodstream, during labour. An inquest concluded that neglect had contributed to the infant's death.
His mother, Robyn, said that "not listening to my concerns is the main reason we're sat here without our son".
Her husband Jonathan believes there is a "cultural" problem within maternity services that midwives believe they know better as they are the professionals. In actual fact, he said, "the only one that truly knows what's going on in that individual's body is the mother".
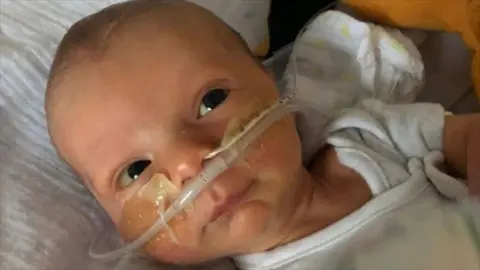 Family handout
Family handoutThe couple are part of a group, Truth for Our Babies, who are campaigning for an independent investigation into maternity services at the University Hospitals Sussex NHS Trust. Earlier this month, BBC News and the New Statesman found that at least 55 babies over a five-year period might have survived with better care.
The Davis family does not believe that the Amos review will lead to better care across England and are calling for a statutory inquiry.
"It's not going deep enough... it's not just what's happening at these hospitals. It's the regulators as well," said Robyn. The regulators are not being reviewed by Baroness Amos.
"As families, we have received lacklustre care," added Jonathan. "We [therefore] deserve the gold standard of accountability - and progressing a rushed, high-level review, instead of a statutory inquiry, is not receiving the gold standard.
"Future mothers and future children may not suffer the same irreversible fate that we have if a [properly] conducted inquiry happens."

Labour MP Michelle Welsh, a prominent campaigner on maternity safety, says there is a danger the Amos review will become a damp squib and is urging the government to act decisively, including creating a maternity commissioner responsible for ensuring care improves.
"This inquiry must result in some big, bold policies with regards to maternity services, that really says that as a government we want to improve maternity services, we want to invest in it, and we will secure the truth and accountability for families," she said.
Announcing the review last June, Streeting also promised that he would chair a maternity taskforce early this year to drive improvements. But it's emerged this week that the group has not yet been established. The Department for Health and Social Care said they would be announcing the membership "shortly".
"It is important that the taskforce is established as soon as possible," said Welsh, "because without it we don't have that driving force [and] those big, bold policies."
