'Trial helps keep me alive after my body rejected donor organs'
 Jonny Humphries/BBC
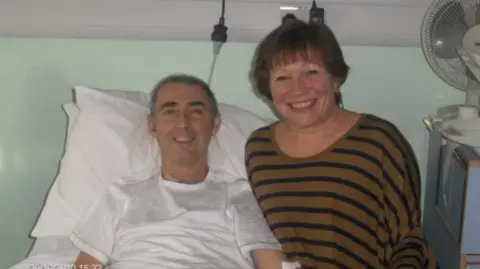
Jonny Humphries/BBCFor Manchester man Steve Cervi, "every day is a blessing" 16 years out from the double lung and heart transplant that saved his life.
But the now 71-year-old has new reasons to be grateful after a medical research trial appears to have stopped or drastically slowed the imminent failure of his donor lungs.
Despite more than a decade of good health, about three years ago he began to show signs of a condition known as chronic lung allograft dysfunction (CLAD), caused by his immune system attacking the donor organs.
After an experimental course of treatment to calm his immune system, the trial funded by the National Institute for Health and Care Research (NIHR) might have extended his life.
He told the BBC: "I'm very grateful and it's not just me that it's touched - it's my family as well."
Before his health problems, the retired engineer, originally from Ancoats in Manchester but now living in Charlesworth near Glossop, was a keen runner who prided himself on his physical fitness.
In 2007, while training with a friend from work, he noticed he was struggling to run a mile and was becoming increasingly breathless.
 Steve Cervi
Steve CerviThe diagnosis was a progressive condition called idiopathic pulmonary fibrosis - a terminal disease which causes irreversible scarring of the lungs.
"Your world just falls apart," Steve said.
"You know when someone tells you that you're dying, and there's no cure, you know it's terminal, it's devastating."
Over the next couple of years, Steve and his wife Lynne were told his only hope was a lung transplant and he was referred to Wythenshawe Hospital's transplant unit.
But the day he was due to be added to the transplant list, he was given more bad news by his doctor.
"They told me 'no, we found the problem with your heart and you'll die on the table'," he said.
 Jonny Humphries/BBC
Jonny Humphries/BBCTests had revealed Steve also had cardiomyopathy, a disease of the heart muscle affecting its ability to pump blood around the body.
Despite that crushing blow, Steve said he was determined "not to be sent home to die" and pushed for more options.
New hope emerged in 2010 when he was referred to the Royal Papworth Hospital in Cambridge, a national specialist in heart and lung treatment.
Surgeons there said they would be willing to take the risk involved in giving him a new lung and would "worry about your heart later".
He said there was a moment of agonising false hope, when he was told an organ was available and rushed by ambulance from Derbyshire to Cambridge - only to be told the donor lung had hardened and become unusable.
But in October 2010, again he got the call he had been waiting for and made the same journey under blue lights.
There were more shocks, this time positive, when Steve was told due to a lack of suitable recipients the donor's other lung and heart were also available.
 Steve Cervi
Steve CerviIn the end, Steve was wheeled into theatre for a surgery performed on average only nine times a year in the UK.
"To be honest I wasn't expecting to wake up again," he said.
"But I wake up and it's like, in this drunken state, 'I'm alive, I've been done'. Just amazing."
Two years after that surgery, Steve managed to run the Great Manchester 10km Run, which he completed three years in a row raising money for charity and in memory of his 18-year-old donor.
Fighting back tears, he said: "You see everything sort of different.
"Just the fact that my son's in Australia and his girls, my grandchildren, are out there.
"You just know that you're going to see them grow up, whereas before? You don't think that."
 Steve Cervi
Steve CerviWith the transplant, however, came the knowledge that at any time he could experience organ rejection.
More than half of all lung transplant patients experience CLAD within five years, and only a tiny fraction are able to undergo another transplant.
Although Steve fared better than many fellow patients, things began to deteriorate about three years ago.
"I just started finding it just a little bit hard to go up and down the stairs," he said.
"I'd stopped running by then but living up here, everywhere you go there's a hill. So I could feel it, going for a walk on the hills and it was at that point it was like there's something not right here."
His fears were confirmed by the team at Papworth who told him his body was rejecting the donor lungs - and the prognosis was measured in months.
Comparing the news with his original diagnosis, he said: "I'd probably come to terms with it a bit more than I had at that point in my life.
"You are prepared for it, you know in the back of your mind it's gonna catch up with you at some point."
 Steve Cervi
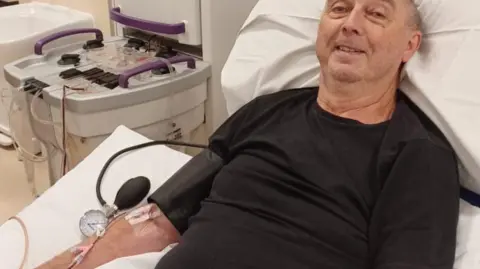
Steve CerviHowever there was one more roll of the dice, his doctors told him - the ongoing trial known as E-CLAD, designed by researchers at Newcastle University with £2m in grants from the NIHR.
The treatment being tested involves repurposing extracorporeal photopheresis (ECP) machines, usually used in the UK to treat blood disorders like leukemia.
In patients like Steve, the machines had been used elsewhere in the world to separate the white blood cells from the blood and treat them with ultraviolet light before returning them to the body.
This calms the body's own defence system, slowing and possibly stopping the progression of CLAD, although it cannot repair any damage already done.
For Steve, while he cannot run any more, he still lives an active retirement and enjoys walking, drawing, building model aeroplanes and trips to the local pub.
"I'm still here with my wife and we have each other," he said.
 Steve Cervi
Steve CerviSteve said his son, Angelo, and his teenage granddaughters visited from Australia last year.
"It means we can just keep planning ahead like that."
Dr Dharmic Suresh, a senior transplant fellow at Wythenshawe Hospital and associate principal investigator for the E-CLAD trial site, told the BBC slowing the progression of CLAD could have a big impact on the lives of lung transplant patients.
"Currently there's no particular magical drug or any treatment to even stop the progression [of CLAD], that's the sad state of it", he said.
"So in that case even if this slows down the progression, it's about increasing their lifespan.
"But also more than that - we also look at other factors like how it can improve the quality of life."
He said early signs in the trial, which is about halfway through, were "promising".
Listen to the best of BBC Radio Manchester on Sounds and follow BBC Manchester on Facebook, X, and Instagram. You can also send story ideas via Whatsapp to 0808 100 2230.
