'Doctors said my excruciating period pain was anxiety'
 Amy Peckham-Driver
Amy Peckham-DriverAmy Peckham-Driver was 14 when excruciating period pains caused her to pass out in a toilet.
She asked doctors if it could be endometriosis, but was told she was too young and was given the contraceptive pill to ease the pain.
Over the next decade, she battled with debilitating symptoms until she was finally diagnosed with the incurable condition, which affects more than 1.5 million women in the UK.
The average waiting time for a diagnosis has now reached nine years and four months, according to a new report by the charity Endometriosis UK.
It found 39% of respondents had to visit their GP 10 or more times before endometriosis was suspected, while 46% of respondents who attended hospital were sent home without treatment.
'My pelvis looked like a bomb had gone off'
Amy, 31, from Needham Market, Suffolk, says she was told her pain must be down to irritable bowel syndrome (IBS) or anxiety. She feels like she was "medically gaslit".
"You know your health is disintegrating in front of you and there's absolutely nothing you can do to stop it, apart from being told to just take the contraceptive pill so you don't have periods."
At 27, she was finally diagnosed with deep infiltrating endometriosis affecting all her pelvic organs.
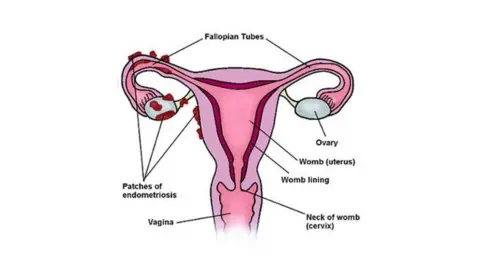
The condition occurs when cells similar to those in the lining of the womb grow elsewhere in the body.
It affects about one in 10 women in the UK and can cause severe pelvic pain, heavy periods, difficulty getting pregnant, fatigue, low mood and pain during or after sex and when going to the toilet.
Amy has had surgery, which she paid for privately due to the long NHS waiting lists, with the surgeon remarking that her pelvis "looked like a bomb had gone off" inside.
Despite this procedure, the endometriosis continues to grow inside Amy.
 Amy Peckham-Driver
Amy Peckham-DriverAmy froze her eggs a few years ago and was told she would need IVF.
But she says when she and her partner applied for IVF several months ago, they were rejected as her egg supply was too low due to her previous surgeries.
"That feels like the ultimate slap in the face because the NHS inadvertently caused my infertility," she says.
"I never would have ended up in that position if I'd been diagnosed 10 years ago."
Amy is now at risk of bowel obstruction and possible kidney failure and is considered an urgent case but remains stuck on a surgery waiting list and feels like she has been "left to rot".
She wants GPs better trained to recognise symptoms sooner, and more research into the condition, stressing it is "not as simple as just having a tummy ache here and there".
A spokesperson for the NHS said the experiences of many women with endometriosis "aren't good enough", with many "waiting for too long before they get adequate diagnosis and treatment".
The NHS was supporting local areas to roll out better and more convenient services, they said.
'The pain was so bad I had to leave my job'
 Ami Clarke
Ami ClarkeAmi Clarke, 28, from Leighton Buzzard, Bedfordshire, started experiencing endometriosis symptoms aged 13 but was not diagnosed until a decade later.
In "unbearable pain" for up to 18 days a month, she kept going back to her GP.
"When I was 18, they said to me 'You could try getting pregnant to see if it helps', which was incredibly disheartening," she says.
Ami tried six different contraceptive pills, but nothing relieved the pain.
"My mental health was terrible. I got an office job but I couldn't focus because I was in so much pain, and I had to leave after 10 months."
When she was 23, she had the Mirena coil fitted, which reduced the amount of bleeding but not the pain.
 Ami Clarke
Ami ClarkeIn 2021, Ami had her first laparoscopy – a surgical procedure using a small camera, which the surgeon can use to diagnose endometriosis and remove some scar tissue.
It reduced the pain for several months, before it returned. Last May, she paid £10,000 for private robotic surgery.
"I have improved so much but I know it's temporary because the endometriosis keeps growing back, so I'm already saving for another surgery," she says.
Ami wants to change the perception of endometriosis and for people to understand it is a "full-body inflammatory disease" rather than just "painful periods".
'My children are watching me deteriorate'
 Faye Ramsey
Faye RamseyEleven years ago, Faye Ramsey, 31, from Ipswich, collapsed with severe stomach pain at a wedding.
Doctors said it was IBS or stress, insisting it could not be endometriosis because it often causes infertility and she had two children.
She was given various contraceptives to ease the pain but they did not help.
Last March, Faye had a laparoscopy and says before the procedure, her surgeon said: "I can't wait for you to wake up and me tell you that I didn't find anything because we're not going to find endometriosis."
Faye was reduced to tears but says she did not challenge him because she felt "my life is going to be in his hands in a matter of hours".
 Endometriosis UK
Endometriosis UKAfterwards, the surgeon admitted he did find endometriosis, but claimed it was "only a small patch" that had been removed and she would be "absolutely fine" now.
Later scans revealed there was still endometriosis with adhesions on her bowels.
"My children are watching me deteriorate. I've not really got that much energy any more," she says.
"It's horrible to feel like you're not doing good enough for your children."
Faye wants education about the condition in schools for both boys and girls, and for doctors to do more than issue contraceptives.
She is also collecting women's health stories to take to the government and says she "will not stop" until she can speak to the health secretary to press for help and changes.
'It took 27 years for me to be diagnosed'
 Mairead Morgan
Mairead MorganMairead Morgan, who is from Omagh, County Tyrone, but lives in Manningtree, Essex, started experiencing symptoms at the age of 11 but was not diagnosed until she was 38.
Now 41, she has moved around the UK for work and feels like she was "back to square one" with doctors each time.
After having a ruptured cyst, she had a laparoscopy to remove some endometriosis, which eased her symptoms for a while, but she still experiences severe pain during flare-ups.
Mairead, an architectural technologist, finds that yoga and cold water swimming help but still has days where she is bedbound and her symptoms have been made worse by perimenopause.
"It has definitely affected my career but as a very ambitious and driven Irish woman, I've powered through," she says.
"You can be fine one minute and in debilitating pain, almost needing hospital intervention, within a few days."
 Mairead Morgan
Mairead MorganEmma Cox, chief executive of Endometriosis UK, says endometriosis care has been neglected for too long, with women enduring years of pain and uncertainty, and that the situation is getting worse.
"Our findings underscore the urgent need not only for increased awareness and understanding of endometriosis and menstrual health among healthcare providers, but for this to be translated into action," she says.
"Governments across the UK must treat endometriosis as a common, chronic condition that requires systematic action and we want an unequivocal commitment to reduce average diagnosis time to one year or less by 2030."
A spokesperson for the NHS said: "Medical professionals, including GPs, should follow NICE (National Institute for Health and Care Excellence) guidelines to diagnose endometriosis – struggling patients can also receive specialist care for menstrual problems and endometriosis through women's health hubs, which are available in most areas."

Get our flagship newsletter with all the headlines you need to start the day. Sign up here.
Follow Suffolk news on BBC Sounds, Facebook, Instagram and X.
