I'm in agony six years after treatment for anal cancer
 Trish Prosser
Trish ProsserA woman diagnosed with anal cancer has said she thought she was going to die after being left in agony following pelvic radiotherapy treatment.
Trish Prosser, 57, said her vaginal walls closed over and she is still dealing with the pain six years on.
The mum-of-four said she was too embarrassed to tell loved ones about the type of cancer she had as she felt there was a stigma surrounding anal cancer.
Anal cancer is rare, with about 1,500 people diagnosed in the UK each year, and approximately 40-50 of those cases are from Northern Ireland.
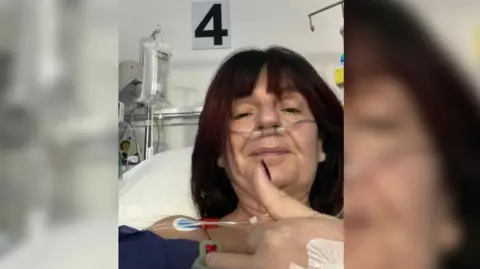 Trish Prosser
Trish Prosser"People are too embarrassed to talk about issues down below or in their bottoms, it can be embarrassing even taboo, but I want to help break the stigma," Trish said.
Being diagnosed in 2020 at the start of the coronavirus pandemic, Trish said it was a lonely cancer journey and it's only recently that she can talk about the trauma.
"I may have looked normal on the outside as I didn't lose my hair, but I felt awful on the inside, I just felt I was falling apart," she said.
"My worst symptom was fatigue; I was so tired. I also had an itch around my anal area, but I had no changes to my bowel habits and to be honest none of those symptoms normally associated with cancer," Trish said.
 Trish Prosser
Trish ProsserUnlike the rest of the UK, Northern Ireland doesn't have a clinic or one-stop-shop for patients who have had pelvic radiotherapy.
According to Trish, who is from Belfast, surviving treatment is just the first stage in a recovery programme which, for many, can take years.
"There are the physical scars which for those who have pelvic radiotherapy can mean dealing with bowel, vulva, cervical and vaginal scarring which is horrendously painful," she said.
"I didn't want people to know what I was going through because it was such a personal area of my body - so when people asked, I just said I'm fine."
What is anal cancer?
Anal cancer is primarily caused by persistent infection with high-risk strains of the Human Papillomavirus (HPV), which accounts for up to 90% of cases.
HPV causes cells in the anal canal to grow abnormally and form tumours.
Other significant risk factors include having a weakened immune system or perhaps a history of other gynaecological cancers.
However, only a tiny proportion of patients with HPV will develop cancer.
 Trish Prosser
Trish ProsserCan pelvic radiotherapy affect intimacy?
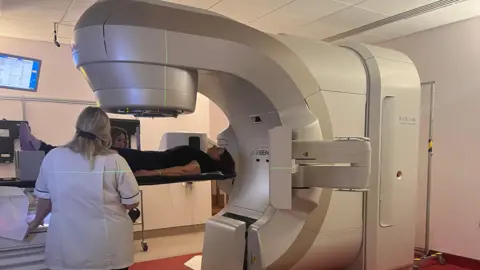
Pelvic radiotherapy for anal cancer can cause significant, long-term vaginal damage due to the proximity of the vaginal tissues to the treatment area.
This condition, often termed radiation-induced vaginal stenosis, involves the development of scar tissue that makes the vagina shorter, narrower, drier, and less flexible which can trigger cuts and damage to the tissue.
While this can happen during treatment, it often becomes a long-term issue month or years after treatment concludes.
"I wasn't aware that my vagina had actually stuck together and I needed to open it again and that had to be done through a dilator or intimacy - and intimacy was painful," Trish said.
"But as you start to recover you start to think about being intimate again and I was so lucky to have a strong loving partner that was patient and helped me through that stage," Trish said.
 Trish Prosser
Trish ProsserCare beyond treatment
Radiotherapy UK with the GI clinical oncology team at the Belfast Health and Social Care Trust have said they want to start a conversation on what is regarded as one of the most under-talked-about cancers.
The aim among charities and clinicians is to create a full care pathway through and beyond cancer.
Sarah Quinlan, of Radiotherapy UK, said: "Late effects from cancer can emerge months or even years after treatment finishes, significantly affecting quality of life, independence and a person's well-being.
"We want a well-resourced, multidisciplinary late effects service so patients don't feel forgotten about after their treatment ends."
Trish is, similarly, calling for a clinic to deal with the after-effects of pelvic radiotherapy.
"During my treatment, my GP was a lifeline, kind and willing to help. But after the treatment ended it became painfully clear that the system wasn't built to support the complexity of long-term side effects associated with pelvic radiotherapy and I was left to navigate everything alone," Trish said.
She said coping with incontinence pads, nappies and dilators designed to stretch vaginal tissue was all "devastating".
"My stomach became so swollen from chronic constipation and weight gain that when I looked in the mirror I was looking at someone I no longer recognised," Trish said.
Physical and mental scars
This weekend, for the first time in Northern Ireland, patients, clinicians, and charities are hosting an event dedicated entirely to anal cancer awareness.
Alison Irwin, a clinical nurse specialist at the Belfast Cancer Centre, is usually the first point of contact for patients after treatment.
"It's all about giving them the words and terminology to break the stigma including telling their family and their employer about anal cancer," she said.
"It's vital that patients feel they can open up to us and tell us everything about their bodies; I have heard it all before, so my relationship with the patient is important," Irwin said.

Dr Catherine Hanna, a consultant clinical oncologist at the Belfast Health Trust, said anal cancer is treatable - with radiotherapy - if diagnosed early.
"It is a rare cancer, and people should look out for a lump in the area, itching and even bleeding.
"If someone is noticing something different in their body, they should get it checked out," she said.
