Our skin is falling off and no-one can tell us why
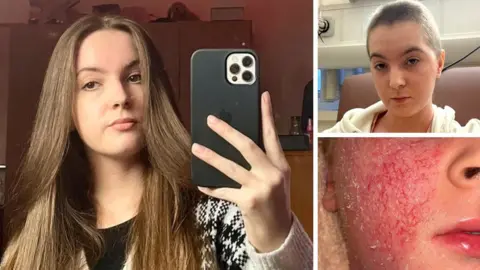 Bethany Gamble
Bethany GambleBethany Gamble was given steroid creams from the age of two to help manage her eczema. They worked - for years her skin condition was just a small part of her life.
And then, suddenly it wasn't.
At the age of 18, Bethany began to notice the small patches of eczema in the creases of her elbows and behind her knees were spreading.
"My skin was hot, so inflamed and red. It began to crack and ooze, and the itch was bone deep. It consumed my whole body, and then it began to consume my whole life."
By the time she turned 20, Bethany was in so much pain she could not get out of bed. She couldn't feed herself and her mum had to take time off work to nurse her.
But the worst part, Bethany says, was not being believed.
"I was constantly gaslit by doctors," the 21-year-old from Birmingham says. "They kept telling me it was just my eczema and offering me more steroids.
"I've had eczema my whole life - this was different."
Bethany is one of a growing number of people documenting their experiences on social media, using the hashtag TSW, which stands for topical steroid withdrawal. #TSW videos on TikTok have been viewed more than a billion times.
Otherwise known as red skin syndrome, TSW is still so under-researched that some GPs and dermatologists struggle to diagnose or treat it.
There are experts who believe it is a debilitating reaction to steroid creams - the first-line treatment for many of the eight million people who have eczema in the UK. Others believe it is itself a severe flare-up of eczema, or other specific skin conditions, and are not convinced it exists at all.
While TSW is viewed as relatively rare, the growing chorus of people on socials sharing pictures and accounts of red, inflamed, peeling skin all over their bodies has triggered the first research of its kind in the UK.
Professor Sara Brown, a consultant dermatologist at the University of Edinburgh, has been so moved by the "unexplainable" symptoms in her own patients and the desperation in the posts on her feeds, she has successfully secured funding from the National Eczema Society to look into what's going on.
"We're seeing patterns in TSW that cannot be explained by what is known about eczema," she says. "Symptoms like thickening and laxity of the skin, so-called 'elephant skin', extreme shedding and sharply defined areas of redness next to normal skin."
She and her co-researcher Dr Alice Burleigh from Scratch That, a TSW patient group, have recruited hundreds of people across the UK to take part in the study - and they're analysing symptoms, saliva samples and skin biopsies to try to figure out why some people get TSW and others do not.
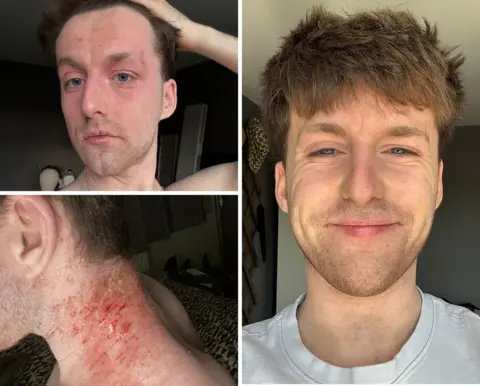 Henry Jones
Henry JonesHenry Jones, 22, from High Wycombe, is one of those taking part in the research - and is among the growing number of people reporting symptoms. He describes himself as a "TSW warrior" such is his determination to raise awareness about the condition.
He says he went from being a teenager who used steroid creams to manage his eczema "every now and then", to experiencing such horrific symptoms he had to drop out of his degree.
"My GP at university kept telling me it was just eczema – and kept prescribing me more steroid cream. Something didn't feel right."
Henry says the more cream that went on, the worse he felt.
"I was so red, my skin was so tight, then it would flake, then it would ooze, and then the cycle would begin again."
As the patches of eczema spread across his entire body, it hurt to move and he could no longer go outside, socialise or study. He says at points he wanted to take his own life.
"My world," Henry says, "became a dark hole caused by the weight of my skin."
- If you have been affected by any issues raised in this article, please visit BBC Action Line
As with many skin conditions, TSW can manifest differently with different skin colours. On white skin it glows an intense red, but on black or brown skin it can appear as deep purple, brown, or with a greyish tinge, which often makes it even harder to spot and diagnose.
 Karishma Leckraz
Karishma LeckrazKarishma Leckraz, from Kent, says she spent many years in denial, convinced this could not be happening to her because it looked markedly different to the posts from white people she had seen on socials.
"TSW took everything away from me. I had to hide from the world for so long. My skin was so bad, the pain, the lack of sleep, just not recognising myself," she explains.
The 32-year-old decided to stop using steroid creams five years ago and says that since then her skin has mainly healed, but she still struggles mentally.
"My social anxiety is huge."
Andrew Procter, from the National Eczema Society, says that while steroid creams can still be very effective for the majority, patients are "stuck between a rock and a hard place".
"We know that steroids work for the many millions who use them. But we also have a condition that at the moment, can't be explained, which is causing real fear - and that is completely understandable. That is why more research is desperately needed."
For those with TSW-like symptoms already facing challenges with anxiety and confusion about what condition they have, getting treatment can pose another obstacle.
GPs may refer patients to dermatologists for more specialist care but there are long waits, often more than a year. For the majority, steroid creams are often the only option available.
At the Royal London hospital, consultant dermatologist Dr Alia Ahmed runs a specialist NHS clinic for people with chronic skin disease, offering options including psychological support, immunosuppresants and phototherapy, which aim to reduce inflammation and calm the body's immune response.
"The psychological impact, as well as the physical effects, is huge," says Dr Ahmed, who is a member of the British Association of Dermatologists. "We have to work with the patient to understand the best course of treatment for them."
 Rebecca Ebbage
Rebecca EbbageThe Medicines and Health Regulatory Authority (MHRA), the UK medicines watchdog, officially recognised TSW as a severe reaction to steroid creams in 2021, but it believes the condition is still relatively rare.
It warns that long-term use of steroid creams can lead to serious side effects such as thinning of the skin, adrenal suppression, or very rarely Cushing's syndrome - a rare disorder caused by prolonged exposure to high cortisol levels through steroids.
Manufacturers now use different ratings on the labels of the creams - from mild to very potent - so there is more clarity on the strength of these medications.
The Royal College of GPs says steroid creams are a "safe and effective treatment for many skin conditions", but in "rare cases" people may experience reactions linked to "long-term or inappropriate use". It recommends patients speak to their GP if they are worried about their treatment and not to stop medication without medical advice.
Rebecca Ebbage, 32, says the day she started showing TSW symptoms was the day her skin became her "ruler". She stopped taking topical and oral steroids in July 2022 after they sent her into a huge flare.
"My skin governs what I am allowed to do," Rebecca says, "what I can eat and even what I can wear - and whether I can leave the house."
After waiting a year for a dermatologist appointment she was prescribed several different immunosuppressants and took them over the course of 18 months, but says, "nothing was working".
"Fight to be believed"
In the end, Rebecca decided to look elsewhere and began to fundraise to pay for treatment - costing £180 per session - at one of a few private clinics in the UK which provides Cold Atmospheric Plasma (CAP) therapy. It is a relatively new therapy - not officially recognised by the NHS - which uses charged gas particles to help reduce inflammation and kill bacteria on the skin in an attempt to speed up the healing process.
After nearly a year of CAP therapy, Rebecca says she is now starting to recover, but stresses that it's not a cure.
Meanwhile, after three years of suffering Henry is under the care of a TSW specialist at the Royal London having finally received an official diagnosis in August 2025. He is taking immunosuppressants and finally feeling "normal again".
After barely being able to recognise herself, Karishma is now the face of various marketing campaigns to raise awareness about debilitating skin conditions and appears on social media and billboards.
"I've spoken to thousands of people around the world about their skin condition," she says. "I don't want anyone to go through what I have gone through."
After years of struggling, Bethany is taking biologics, a relatively new type of medication which targets inflammation, has recently secured her first job and feels she's finally getting her "life back".
At times in the past, she says, she'd have been tempted to punch anyone who told her to "just stop scratching".
Now her message to anyone suffering as she once did is clear.
"Do not feel guilty, do not feel like it's your fault- and fight to be believed."
